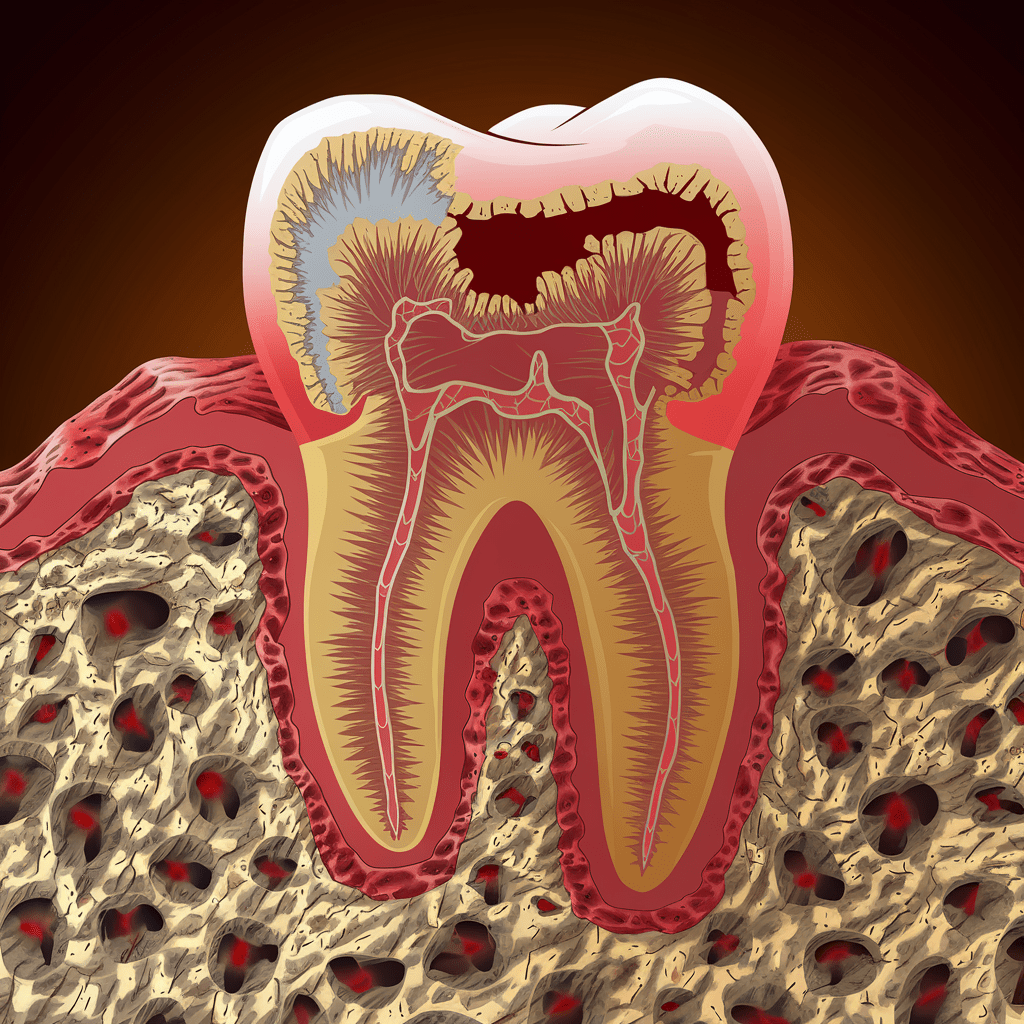
Tooth resorption is a complex dental condition that can perplex many patients and even some professionals due to its subtle onset and varying causes. Essentially, it refers to the breakdown and loss of the tooth’s structure, including its outer enamel, inner dentin, and sometimes even the root itself. Understanding why tooth resorption occurs is key to early detection and prevention of irreversible damage. Let’s dive deep into the root causes and explore how this condition develops.
What Is Tooth Resorption?
Tooth resorption is the process by which the body begins to break down and absorb the tooth structure, either from the inside (internal resorption) or the outside (external resorption). This can happen to both the crown and the root of a tooth. While it’s a natural part of losing baby teeth, in adults, it’s a pathological process that leads to tooth damage and potential tooth loss if left untreated.
Prevention of Tooth Resorption
While some causes of tooth resorption, such as genetics, cannot be prevented, maintaining good oral hygiene and attending regular dental check-ups can help reduce the risk. Avoiding excessive stress on the teeth, such as bruxism, and managing conditions like gum disease are also important steps in prevention.
For a more in-depth exploration of tooth resorption, including expert advice and treatment options, you can visit here. This resource provides comprehensive insights into the causes, diagnosis, and treatments of tooth resorption, helping patients understand their condition and seek timely dental care. Whether you’re dealing with symptoms or just want to learn more, visiting this link will guide you through everything you need to know about tooth resorption.
Types of Tooth Resorption
There are two main types of tooth resorption:
Internal Resorption
Internal resorption occurs when the dentin (inner part of the tooth) begins to be absorbed from the inside out. This often leads to a hollow appearance within the tooth, and the patient may notice a pinkish hue due to the enlarged pulp chamber. It is a rare occurrence but requires immediate attention once identified.
External Resorption
External resorption, on the other hand, starts from the outside and progresses inward. This type is more common and can affect the roots, causing them to shorten. If not detected early, external resorption can lead to severe damage and even tooth loss.
The Underlying Causes of Tooth Resorption
Understanding the causes of tooth resorption is crucial for both prevention and treatment. Several factors contribute to this condition, and each plays a different role depending on whether the resorption is internal or external.
Trauma and Injuries
One of the primary causes of tooth resorption is trauma or injury to the tooth. Physical trauma can trigger the body to start reabsorbing the tooth tissue, mistaking it as something foreign or damaged. This could be due to a direct blow, such as a sports injury or accident, or even due to chronic grinding or clenching of the teeth (bruxism).
Orthodontic Treatments
While braces and other orthodontic appliances are essential for correcting misalignments, they can also exert pressure on the teeth and roots, leading to resorption in some cases. The constant pressure applied to move teeth can occasionally cause the body to resorb the root structure, particularly if the force is excessive.
Chronic Inflammation and Infection
Inflammation, especially if it becomes chronic, is a significant factor in tooth resorption. When gums and surrounding tissues become infected, the body’s immune response can inadvertently target the tooth structure, leading to resorption. This is often seen in cases of untreated periodontal disease or pulp infections.
Genetics and Family History
Genetics can also play a role in the development of tooth resorption. Individuals with a family history of resorption are more likely to experience it themselves. While this factor is not within one’s control, awareness of genetic predispositions can help patients and dentists stay vigilant.
Teeth Grinding (Bruxism)
Bruxism, or the grinding and clenching of teeth, can put excessive stress on the roots and lead to resorption over time. The constant pressure wears down the protective layers of the tooth and can lead to both internal and external resorption if the habit persists.
Hormonal Changes
Hormonal imbalances, particularly those that occur during pregnancy, menopause, or due to conditions like hyperthyroidism, can influence the occurrence of tooth resorption. The fluctuation in hormones can weaken the tooth’s structure and make it more susceptible to resorption.
Resorption Due to Cysts or Tumors
In some cases, resorption occurs as a result of cysts or tumors developing near the tooth. These growths put pressure on the surrounding teeth, causing the roots or the crown to resorb over time. This is an uncommon cause but should be considered when evaluating the root causes of tooth resorption.
Symptoms of Tooth Resorption
Tooth resorption can be asymptomatic in its early stages, making it difficult to diagnose without a dental examination. However, as the condition progresses, patients may experience:
- Pain or discomfort
- A change in the color of the tooth (often pinkish or darkening)
- Loose teeth
- Swelling or sensitivity around the affected area
- Visible damage to the tooth structure
Diagnosis and Detection of Tooth Resorption
Early detection of tooth resorption is critical to preventing permanent damage. Dentists typically use X-rays and other imaging techniques to identify the extent of the resorption. Regular dental check-ups are essential for catching resorption early, as it often develops without noticeable symptoms.
Treatment Options for Tooth Resorption
The treatment for tooth resorption depends on the severity and type of the condition. If detected early, it may be possible to halt the resorption process and save the tooth. Options include:
- Endodontic therapy (root canal): Particularly for internal resorption, root canal treatment may be necessary to remove the inflamed pulp and protect the tooth from further damage.
- Surgical intervention: In cases of external resorption, surgery may be required to remove the damaged parts and restore tooth function.
- Tooth extraction: If the damage is too severe, tooth extraction may be the only option.
When to See a Dentist
It’s essential to see a dentist as soon as you suspect any abnormal changes in your teeth. Early diagnosis and intervention can prevent tooth resorption from causing irreversible damage, saving you from tooth loss and other complications. If you experience any signs of resorption or have concerns about your dental health, don’t hesitate to seek professional help.
FAQs
Q1: What is tooth resorption?
Tooth resorption is a dental condition where the body breaks down and absorbs the tooth’s structure, including the enamel, dentin, and roots.
Q2: What are the main types of tooth resorption?
There are two types of tooth resorption: internal resorption (from the inside out) and external resorption (from the outside in).
Q3: Can tooth resorption be reversed?
Once tooth resorption begins, it cannot be reversed, but early detection can help manage the condition and prevent further damage.
Q4: How is tooth resorption diagnosed?
Tooth resorption is typically diagnosed through dental imaging, such as X-rays, during a routine dental check-up.
Q5: What causes external tooth resorption?
External tooth resorption can be caused by trauma, orthodontic treatments, infections, or pressure from cysts or tumors.
Q6: Is tooth resorption painful?
Tooth resorption can be painless in its early stages but may cause pain or discomfort as the condition progresses.
Q7: How common is internal tooth resorption?
Internal tooth resorption is rare compared to external resorption but requires prompt treatment once identified.
Q8: Can genetics cause tooth resorption?
Yes, genetics can play a role in predisposing individuals to tooth resorption.
Q9: How can tooth resorption be prevented?
Preventing tooth resorption involves maintaining good oral hygiene, attending regular dental check-ups, and avoiding excessive tooth stress, like grinding.
Q10: What are the treatment options for tooth resorption?
Treatment options include root canal therapy, surgical intervention, or, in severe cases, tooth extraction.